
Anne Rogers and Gerry Nicolaas (1998) 'Understanding the Patterns and Processes of Primary Care Use: A Combined Quantitative and Qualitative Approach'
Sociological Research Online, vol. 3, no. 4, <http://www.socresonline.org.uk/3/4/5.html>
To cite articles published in Sociological Research Online, please reference the above information and include paragraph numbers if necessary
Received: 05/08/98 Accepted: 15/12/98 Published: 31/12/98
 Abstract
AbstractThe study conducted in three different areas in the North west of England was designed to, link health status to subsequent use of health care in a way which might be used for service planning and the allocation of resources, and to provide data to inform a long term programme examining the relationship between need and demand for primary care. The study was in two stages, a survey and diary study designed to ascertain frequency of health care utilisation and health status of households, followed by a linked qualitative study consisting of in-depth interviews on a subset of people experiencing a range of common complaints seen in primary care. The mixture of methodologies gave a broader understanding of the dynamics of health utilisation in the localities studied. The survey and diary data showed the way in which key variables can be used to map the patterns of primary care utilisation in a population and the extent of self care actions and lay management of illness undertaken within households. We found that ill people are far more likely to use self care than professional health care services, and when they do use formal services, this tends to be in addition to self care practices. The qualitative data illuminated more about the processes of health care utilisation, particularly the way in which the past experience of illness and service contact coalesced with peoples' more immediate decision making about using primary care services. The findings suggest that health care use is most appropriately viewed as an interplay between agency and structure rather than the outcome of 'expressed need', individual decision making or 'supply induced' demand.
 Introduction
Introduction
 Combining Qualitative And Quantitative Methods
Combining Qualitative And Quantitative Methods
 Design And Methods
Design And Methods
| Area A:-a deprived, predominantly white, urban area |
| Area B: -a socially mixed urban area |
| Area C: -an affluent semi-rural area with a large elderly population |
 Survey And Diary: Results And Discussion
Survey And Diary: Results And Discussion
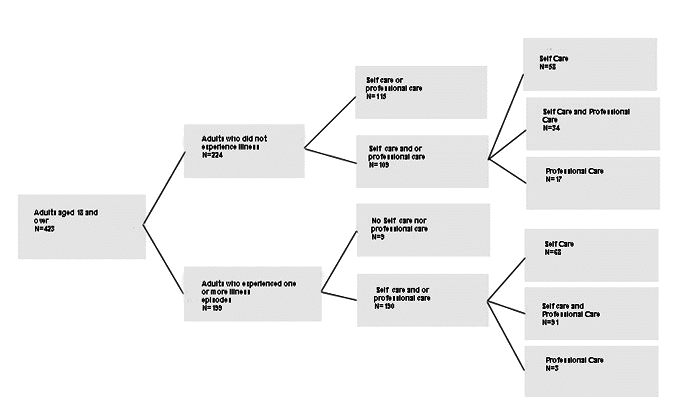
| I: "Does he try to treat himself, or get any home remedies or do anything to make himself feel better, apart from what he gets from the doctor?" |
| R:"erm no not really, just on the prescription from the doctor. It's permanent all the time" |
| I:"What does he have?" |
| R:" just pain killers and anti-inflammatories" |
| I: "And how often does he go to the doctors your husband?" |
| R: "... Only when he needs to for prescriptions I just get a repeat, I just take it in" |
| I: "Oh so doesn't he have to see his doctor regularly?" |
| R: "No" |
| I: "And what..?" |
| R: "Well actually he has got to go because he's got a form off the doctor, so in the next couple of weeks he'll be going." |
| I: "Is that just like normal." |
| R:"Just to see how he is- about once a year" |
| I:"But apart from that he does he go ?" |
| R: "No unless like I say he's just got laryngitis so he's just been twice." |
Thus service use was in response to short term need with only residual attention being given to this mans' main and long term health problems.
Mrs B is a 74 year old widowed woman with multiple health problems including a history of back pain, breathing difficulties, heart disease and high blood pressure. Data from the diary and survey revealed 28 illness days for angina and breathing difficulties but no primary care consultations. Illness action recorded in the diaries included the consumption of prescribed and over the counter medication'.The qualitative account revealed that the illness episode reported in the diaries did lead to consultation immediately after the end of the diary period. According to the woman's account, the extent of her use of primary care for long term health problems was subject to flux, but overall had decreased over time. This quote describes the use of the 'on - off' nature of formal service contact and the not insubstantial part played by the GP in generating demand
"Well when I started with the breathing problem, then they wanted to see me pretty regular. ..... At first I was going once a week and then tailing off to two monthly visits based on doctors recommendation and returns at two monthly intervals."
"Well its usually my hip that bothers me more than anything, but they won't do it if you are overweight."
"I had a bad angina attack and then of course I was confined to the house it takes 3/4 days to get over a bad one, you've just got to rest you can't do anything else really ."
"So I woke up one morning and pain in my back and my leg and I couldn't believe it, its a terrible pain it really is.... I knew my daughter was coming everyday you see which she does most times anyway and she came and she said 'what on earths to do' I said I can't get out of bed....I said the pain is driving me crackers anyway she said, 'oh get the doctor', you see so it was from that she sent for the doctor and he came."
"where I go it's the other end of town. Well if you are fit enough there is no problem but you have to get 2 buses. ..You go into town and then you get one from town onto the road where the medical centre is and then you've to walk across to it. But its the you know getting there (laughs). I mean tomorrow if I had to go to the doctor I'm alright because my daughter comes for me and we go to Quiksave in B."
 Unpredicted Utilisation Of Services - Low Need And High Use?
Unpredicted Utilisation Of Services - Low Need And High Use?
This case illustrates that the level and nature of the service utilisation is linked to a number of complex processes operating at the level of interaction with professionals, prior personal experience of illness, the immediate social context and social networks. During the six week period covered by the survey and diary Mrs C a 40 year old woman in full time paid employment living with husband aged 43 sons of 14 and 4 years of age respectively with no apparent long term limiting illness reported consulting the GP 15 times. Ms C had experienced Colitis once before 6yrs previously. She was also aware of the nature and remedies available for this condition from her sister who also suffered chronically from this complaint. After 4 days of experiencing symptoms she consults the doctor for the first time:
| I:"What finally made you decide to go to the doctors?" |
| R: " realised it wasn't just diarrhoea, but was something different than the runs." |
"Working behind a bar, I couldn't work with the symptoms, serving and I'd thought, oh my God it's coming, it was that bad, once it did come and I though Oh, it's so embarrassing and I nearly died a death..."
"It was like Dr B I asked her for these tablets my sister told me to get and she (the GP) said they will help you but I can't give you them,' ...You see I asked the doctor for these tablets and she said yes they probably will clear it up but you must go to the hospital first to see what it is..."
"And it was still happening, so I was going to the doctors, every time they shouted out it's not her again', I was a mess- a complete mess even at home I was crying and I cried and I cried ......and then they gave me a hospital appointment after three weeks she (the GP) put me on the scales and I'd lost over half a stone and she said 'I'm sorry but I think this is more serious than just the diarrhoea I think we'll have to do something about it', so she got me an appointment but I had to wait seven weeks for that... I said is there no chance you can get me in any earlier' and they said no chance at all' so in the meantime I said have I just got to put up with it?' and they said Yes I'm sorry'. Anyway after seven weeks of having it I went to the hospital and by that time I'd lost one and a half stone..."
"So I saw my sister and she gave me these tablets I was so bad it was Christmas week I was working and I felt so down and I'd lost so much weight, so I thought what harm can it do? I've never done it before take other peoples tablets...I've been smashing since."
"My sister told me about these tablets they gave her when she went to hospital, she had to go private in the end because she was that bad (our emphasis)."
"I daren't tell my doctor, I've not been to the doctor since because I've not had nothing wrong. They (the GP's)were very nice its just that I don't think I seemed to get anywhere with it."
The final case Ms D is a lone parent of 26 years working part time as a cleaner who has a four year old child suffering from asthma. She too suffers from intermittent asthma. The frequent use recorded in the diaries related directly to the material resources available to deal with an illness episode rather than solely to levels of health need. Visits to the doctor are made for exempt' prescriptions (for which no payment is required) to obtain medication which the respondent knows it is possible to obtain over the counter from the chemist. This includes prescriptions for decongestants for herself and Calamine lotion and Calpol for her child:
| I:"Are there times when you go to your chemists rather than your doctors?" |
| R: "No You have to pay at the chemists. ...Well your over the counter stuff it can be expensive can't it you know why pay when you can get it free?" |
"I don't go to the doctors unless I need something so I always do come away with a prescription....you can generally work out what's wrong with yourself anyway can't you?"
 Understanding The Patterns And Process Of Primary Care Utilisation
Understanding The Patterns And Process Of Primary Care Utilisation
 Implications For Combining Methods In Applied Sociological Research
Implications For Combining Methods In Applied Sociological Research
 Conclusion
Conclusion
 Acknowledgements
Acknowledgements
ANDERSON, R. (1995) Revisiting the behaviour model and access to care: does it matter? Journal of Health and Social Behaviour: vol.36.
ARCHER, M . (1996) Social integration and system integrationSociology :vol. 30.
BENTZEN N., CHRISTIANSEN T. and PEDERSEN KM. (1989) Self-care within a model for demand for medical care. Social Science and Medicine: vol.29:2.
BENDELOW, G. (1996) A failure of modern medicine? Lay perspectives of a pain-relief clinic in Modern Medicine:Lay Perspectives and Experiences (eds.) WILLIAMS S and M CALNAN) London: University College London Press,
BLOOR, M (1985) Observations of abortive illness behaviour.Urban Life vol.14 (3).
BRANNEN, J. (1992) Combining qualitative and quantitative methods. An overviewIn J. Brannen (Ed.), Mixing methods: Qualitative and quantitative research. Brookfield,VT:Avebury
BRYMAN, A. (1988) Quantity and quality in social research Boston: Unwin Hyman
CARR-HILL RA., RICE N. and ROLAND MO. (1996) Socio-economic determinants of rates of general practice consultations. British Medical Journal :vol 312.
COWIE, W. (1976) The cardiac patient's perception of his heart attack Social Science and Medicine:vol.10.
CUNNINGHAM -BURLEY, S. And IRVINE,S. (1987) And have you done anything so far ?' An examination of lay treatment of children's symptoms British Medical Journal: vol. 295,
DINGWALL, R. (1976) Aspects of illness London:Martin Robinson
LAURIE, H. and SULLIVAN, 0. (1991) combining quantitative and qualitative methods in the longtitudinal study of household allocations Sociological Review: vol. 39.
MCCORMICK A., FELMING D. and CHARLTON J. (1995) Morbidity Statistics in General Practice: Fourth National Study: 1991-1992. Series HMSO : MB5 no. 3, London.
MECHANIC, D. (1979) Correlates of physician utilization: why do major multi-variate studies of physician utilisation find trivial psychosocial and organisational effects Journal of Health and Social Behaviour vol. 20:
NICOLAAS G, ROGERS A, ELLIOTT, H, CARR-HILL R, ROBERTS C, POPAY J, and WILLIAMS G (1997) Population health, pathways into primary care and the use of health care: Phase 1 a report of reviews Summary Report. Manchester:National Primary Care Research and Development Centre
ONG B.N and JORDAN, K. (1997) Health experiences of elderly people in an outer London area Sociological Research Online 2,1,
PARKIN. D, SUTTON., M and RICE, N. (1998) Changing patters of self-reported health and use of GP services in Great Britain, 1984-1995 paper presented to the health economics study group meetingGalway: July 1998
PESCOSOLIDO, B.A. (1991) Illness carers and network ties: a conceptual mode of utilisation and compliance Advances in Medical Sociology: vol 2.
PESCOSOLIDO, and B.A BOYER, C. (1996) From the community into the treatment system- how people use health services. In the Sociology of Mental Illness (eds A Horwitz and T.Schneid) New York: Oxford University Press.
PESCOSOLIDO, B.A. and KRONENFELD, J. (1995) Health illness and healing in an uncertain era: challenges on, from and for medical sociology Journal of Health and Social Behaviour (extra issue)
ROBINSON, D. (1971) The process of becoming ill London: Routledge Kegan and Paul
ROGERS A, CHAPPLE, A. and HALLIWELL, S. (1998) The influence of paid and unpaid work on help-seeking for primary care Social Sciences in Health: vol.4(3).
ROGERS, A., HASSELL, K. and NICOLAAS, G. (1999) Demanding patients?: analysing primary care use Buckingham Open University Press
ROSENSTOCK, I. (1966) Why people use health services? : Millbank Memorial Fund Quarterly vol.44.
SCHEFF,T. (1997) 'Part/Whole Morphology: Unifying Single Case and Comparative Methods Sociological Research Online vol 2, no.3,
SCHILLING, C. (1997) The undersocialised conception of the embodied agent in modern sociology Sociology: vol.41,4.
SMAJE, C. and LE GRAND, J. (1997) Ethnicity, equity and the use of health services in the British NHS Social Science and Medicine: vol.45, (3).
SILVERMAN, D (1985) Qualitative Methodology and Sociology: Gower
STANLEY, L (1993) On Auto/Biography in Sociology Sociology: vol.27,1.
WADSWORTH, M., BUTTERFIELD, W and BLANEY, R. (1971) Health and sickness: the choice of treatment. Tavistock: London
WHITE K L, WILLIAMS F, GREENBERG B G and HILL C (1961). The ecology of medical care New England Journal of Medicine: vol.265.
WILLIAMS, R. (1983) Concepts of health: an analysis of lay logic Sociology vol.17(2).
WILLIAMS S.J. (1995) Theorising class, health and lifestyles: can Bordieu help us? Sociology of Health and Illness vol.17,5.
WILLMOTT, R. (1997) Structure,culture and agency:rejecting the current orthodoxy of organisation theory Journal for the Theory of Social Behaviour vol. 27.
ZOLA, I. (1973) Pathways to the doctor:from person to patient Social Science and Medicine vol. 7.