'Are My Bones Normal Doctor?' the Role of Technology in Understanding and Communicating Health Risks for Midlife Women
by Eileen Green, Frances Griffiths and Di Thompson
University of Teesside; University of Warwick; University of Hertfordshire
Sociological Research Online, Volume 11, Issue 4,
<http://www.socresonline.org.uk/11/4/green.html>.
Received: 28 Nov 2005 Accepted: 22 Sep 2006 Published: 31 Dec 2006
Abstract
Contemporary medical science is increasingly saturated with risk and uncertainty, uncertainty which health professionals are obliged to manage in everyday consultation situations, but which patients presenting with specific health problems, want resolution to. This paper provides an overview of literature concerning the medicalization of women's bodies via health interventions such as screening, including the role played by medical technologies in defining degrees and forms of risk and uncertainty which are embedded within and generated by the screening processes themselves. We draw upon an ESRC funded study into the use of health technologies in women's midlife, in order to demonstrate how empirical research can illuminate the links between screening for osteoporosis and the recommendation and subsequent decision by women to use therapies such as hormone replacement therapy (HRT).The paper explores the centrality of bone densitometry in decision-making about potential risk. Drawing mainly upon data from 24 consultations in specialist clinics, 10 follow up interviews with the women concerned and 7 interviews with linked health professionals, we focus upon the interpretation and significance of the bone scan results. We conclude that, although the technological results are open to flexible interpretation, they seem to confirm the 'at risk' status of many of the women. The scan results appear to assume centre-stage in the consultation discussions, leading both women and clinicians to over interpret their significance as an indicator of risk.
Keywords: Bone Densitometry, Risk, Midlife Women, Osteoporosis, Technology
Introduction
1.1 Alongside growing concerns about maintaining the health of an increasing elderly population is an expanding literature on the relationship between biology, technology and the social (Webster 2002; Williams, Birke et al. 2003) focusing upon the rise and proliferation of innovative health technologies. This literature critiques the implied promise of new health technologies that have become associated with prolonging active life, and alerts us to the problem of 'over medicalisation' in the normal process of ageing. Similar concerns are highlighted in recent international studies of women and ageing (Gannon 1999; Tannenbaum, Nasmith et al. 2003). Midlife women experiencing or entering menopause are implicated in debates about 'the expanding elderly', debates which sociologists argue, focus upon representations of them as primarily menopausal bodies: emotional, unstable and at risk of being 'out of control,' (Lupton 1998). This representation of older women has been challenged by numerous feminists (Greer, 1991; Coney, 1991; Lock, 1998; Ballard, 2002). Among them Gannon (1999), who observes that the labeling of menopause as a disease, with the associated concept of declining hormones and bone mass as abnormal, ignores the fact that 'women who live to age 75 spend more years in a state of "estrogen deficiency", than they do in a state of "estrogen abundance'(1999: 8), i.e. it is normal. Constructing ageing women as 'abnormal' and a risk to themselves and others, encourages them to engage in what Armstrong (1995) and other sociologists (Burrows et al, 1995; Lupton, 1995) refer to as 'embodied surveillance', which as Howson argues ' heightens and potentially contributes to the development of risk consciousness' (1998a, p196). It also signals the need for intervention to reverse or delay such 'decline and deficiency', not least through intervention from medical technologies such as those involved in screening. Theoretical debates about risk and body management have provided useful conceptual frameworks through which to address women's experiences of ageing. Pivotal to our understanding of such experiences are the ways in which women are represented as bodies that need to be carefully managed, whether it be by medical experts or by themselves, through a mixture of personal care and 'self surveillance'.1.2 The aim of this paper is to explore the role of technology in both the communication of health risks to midlife women and in facilitating their understanding and management of health risk and in particular, the factors behind the elevated status of DEXA scan measurements in decision making. We explore this theme through our focus on an ESRC funded study into the use of health technologies in women's midlife, in order to demonstrate how empirical research can illuminate the links between screening for osteoporosis and the recommendation and subsequent decision by women to use therapies such as hormone replacement (HRT) or bisphosphonates for prevention[1] . First of all this paper will provide an overview of literature concerning the medicalization of women's bodies via health interventions such as screening, including the role played by medical technologies in defining degrees and forms of risk and uncertainty which are embedded within and generated by the screening processes themselves. Second, the paper discusses the methodology adopted and presents data which illustrates the ways in which the communication of screening results influences decisions about treatment. Finally, some implications of different perceptions of osteoporosis risk between health professionals and women patients are considered for health decision making.
Risk and health surveillance
2.1 The study of risk has been of central sociological interest for over a decade. In particular, there can be identified a strand of research that derives from what might be said to be general efforts of modern societies to enhance the health and well-being of their populations and to exert increasing control over our lives and our environments. Developments in science and technology would appear to offer us more opportunities to prevent threats to our health and well-being and allow us more prediction and intervention to curtail harmful future events ( Alaszewski et al. 2000). Traditionally, the focus of biomedicine has been upon the ill patient but as Armstrong (1995) has argued, a new 20th century paradigm blurred the boundaries between the healthy and the diseased, in such a way that the previously discrete categories of symptoms and diseases have become subsumed under a more general category of 'risk factors' that can point to some future health problem.2.2 Contemporary risk theorists (Giddens 1991; Beck 1992) have argued that identity is increasingly articulated through differing dispositions towards risk, among them embodied health risks (Lupton 1999). An expanding body of work has begun to focus upon the ways in which medical culture has contributed to both the generalization of risk and the belief that it can be calculated and eliminated through medical surveillance techniques (Burrows et al 1995). Alongside this, is research which addresses the risks linked to medical technologies themselves, including the role that technology-based images play in the decision making process (Prior, Wood et al. 2002), for example defining degrees of health risk and uncertainties via screening for prevention. The introduction of new technology into biomedicine creates new types of diagnostic and treatment practices, and new definitions of what constitutes 'acceptable risk' are emerging both in healthcare systems and among lay consumers. As the number and variety of health conditions detected via preventative screening increases, so does the imperative for individuals to engage in what Foucault (1973) has referred to as medical surveillance of the body. Early knowledge of potential health risks has become represented as both our 'right to know' and our 'duty to find out', so that they can be avoided. However, as Howson has argued in relation to cervical screening, the experience of screening itself may also re-enforce a sense of 'risk' (1998a p195).
The medicalization of women's bodies through screening
3.1 Howson's work (1998a, 1998b, 1999, 2001) has been influential in drawing attention to both the ways in which screening programmes for prevention are deeply gendered and the absence of gender perspectives within much of the literature on health surveillance and risk (Howson, 1998b and 2001). Research on cervical screening has refined the debate about 'surveillance medicine' (Armstrong, 1995), including highlighting the extent to which disease prevention and health surveillance strategies have tended to target women (Graham, 1979). In addition, some feminist work has developed frameworks for exploring issues of power and gender within different types of screening programmes (Singleton, 1995; Bush, 2000; Reventlow, et al 2005 Griffiths, et al 2005). Particularly pertinent are debates about screening as a key process through which women's bodies become subjected to the 'medical gaze' (Howson 2001). Lock's (1998) research on managing the post menopausal body alerts us to the conceptualisation of midlife women as situated at one of the 'transitional moments, often associated with danger or crises' (p35), a positioning which is implicit in the widespread acceptance of the need for them to engage in medical surveillance in the form of screening for osteoporosis such as bone densitometry. Similarly, in the context of screening, risk is seen as objective and measurable, re-enforcing the premise that midlife women's participation in screening programmes is a rational response to risk.3.2 Despite widespread acceptance by both women and health professionals that it is 'better to go and know' (Richardson et al, 2002) i.e. find out about the state of your bones, closer examination of the screening experience suggests considerable uncertainty and ambiguity around interpretation of the screening results. Howson (2001) and others (Kavanagh and Broom, 1998) point to the tension between different forms of uncertainty associated with the cervical screening process, and women's perceptions of the benefits of 'being checked out'. This research is congruent with our own findings about the uncertainties generated by screening for osteoporosis which are presented later in the paper. Equally pertinent is literature on the disjunction between expert and lay concepts of screening for prevention (Posner and Vessey, 1988; Howson, 1998b), although space limits detailed discussion of it in this paper. Also useful are Howson's observations on the disjunction between the preventative aim of cervical screening programme as understood by health experts and women's lay perception of screening for detection of disease or its absence (Howson 2001, p171), in attempting to interpret differences between lay and expert accounts of bone densitometry screening for osteoporosis.
3.3 Although there are now a number of studies of cervical screening that are informed by social science perspectives, as well as an expanding body of work on women's experience of the menopause and midlife (Martin, 1987; Greer, 1991; Lock, 1998; Griffiths, 1999; Green et al, 2002), and a growing interest in theorising embodied risk (Kavanagh and Broom, 1998; Howson, 1998a); social scientists have paid little attention to screening for osteoporosis. A notable exception is the work of Reventlow and colleagues (2002; 2005) who have explored changes in women's sense of embodied identity after bone scans. Drawing upon such perspectives, in this paper we address women's understandings and experience of bone densitometry screening and that of key health professionals, in an attempt to extend existing conceptual frameworks of health and illness through an exploration of the role of specific screening technologies in health decision -making.
Osteoporosis screening and the construction of risky midlife women
4.1 Osteoporosis or 'thinning of the bones' is a highly publicised health condition, mainly associated with ageing women (Gannon, 1999), that is represented as prevented or 'cured' by treatments such as HRT. Screening for 'thinning bones' via bone densitometry has become increasingly accepted by both women (post and pre-menopausal) and health practitioners (Richardson, Hassell et al. 2002) as a key route to minimizing risks associated with the onset of osteoporosis. The process of DEXA scanning produces images of the bone structure using Xrays whilst measuring bone mineral density. The result is represented in both a picture and a numerical curve graph, which is mapped against the mean within the same age group, as well as that of healthy adults (see Figure 1). Definitions of osteoporosis centre on a decline in bone mineral density to below the expected bone mass for a person's age and sex [2]. Asymptomatic and represented as 'a silent killer', osteoporosis is also widely perceived as a women's disease (Richardson et al, 2002) with a projected one in three women likely to experience a fracture during their lifetime (Royal College of Physicians and Bone and Teeth Society, 2001). This has led to public health initiatives to identify 'high risk' women and increased awareness of osteoporosis among women themselves.4.2 Despite such increased awareness as Reventlow et al argue, developing 'osteoporosis (however) does not necessarily imply that a fracture will occur' (2005, p2) and such heavy emphasis upon prevention encourages current health status to be perceived in relation to future health risk. As we demonstrate in the findings section, a number of women in our study were both keen on discovering their potential risk of osteoporosis via screening, and persuaded that HRT was the best insurance against such risk[3]. Such positive attitudes are connected with the assumption that it is possible to accurately predict individual future risk of osteoporosis and consequences such as hip fracture, and that DEXA scanning provides the technology to achieve it, an assumption which is debatable in biomedical research contexts but which appears to remain opaque in lay contexts. Key components of this debate include the over interpretation of DEXA scan results to infer future risk of fracture from 'low' bone density measurements. Furthermore, as Wilkin et al., (2001) argue, the evidence that bone density levels can predict fracture is based upon epidemiological studies of large populations which cannot be 'read off' for individuals. There are many other factors which may be important indicators but cannot be scientifically measured e.g., diet, life style, genetic inheritance etc. Despite such complexities, bone densitometry technology appears to play a powerful role in the process of health risk prediction and communication. As we demonstrate later in the paper, our data confirms that individual women are closely engaged in risk avoidance and a major dialogue between practitioners and women patients concerns the management or avoidance of health risks. The next section describes the empirical research that the paper draws upon.
The Study
5.1 Part of the ESRC Innovative Health Technologies Programme, the project focused on health technologies and midlife women's health [4], and included collecting data on mammography screening, the use of hormone replacement therapy (HRT) and screening for osteoporosis using bone densitometry.Method
6.1 The data from the wider study[5] informs the analysis presented in this paper; however the focus of the analysis is on the sub-group of data collected in two UK National Health Service clinics where bone densitometry was undertaken or its results discussed. This sub-data set included 24 recorded clinical consultations, 10 interviews with women and 7 interviews with health professionals. A member of the research team attended the clinics for recruitment on a total of five days (1.5 days when women attended for the bone densitometry measurement and 3.5 days when women consulted about abnormal bone densitometry scans). Women within the target age range (45-64 years), attending the clinics on these days, were asked to consent to the recording of their consultation and 24 agreed. The women were also asked for an interview until a total of 10 had agreed. The research team aimed to sample 10 women for each sample subgroup within the whole study. The clinics were staffed by doctors, nurses and radiographers. Seven of these health professionals agreed to interview: 4 doctors, 1 nurse and 2 radiographers. Interviews with health professionals were completed within two weeks of recruitment and interviews with women within six weeks of recruitment.6.2 Collecting data from the three different sources enabled triangulation between the data sets. In addition, although not part of the initial research design, there was some triangulation at an individual level. Four consultations between doctors and women triangulated with individual interviews with those doctors and interviews with the women concerned.
6.3 The women had all been referred for bone densitometry by a health professional, a process which may have affected the women's accounts. From the interviews it was apparent that what was important to the women was the experience of hearing the result of the technological measurement. The analysis presented here focuses on interpretations and perceptions of information from specific women's bone densitometry measurements. This information consists of a computer generated printout of an image of the bones and a table and graph of the density measurement results (hip and spine) in comparison with the 'normal' population. The graph is divided into colour-coded bands with 'normal' measurements indicated by a blue area and 'at risk' measurements outside this area (see Figure 1). The detail is interpreted for the woman by a doctor in a clinical consultation.
Figure 1: Example of a bone densitometry results print out
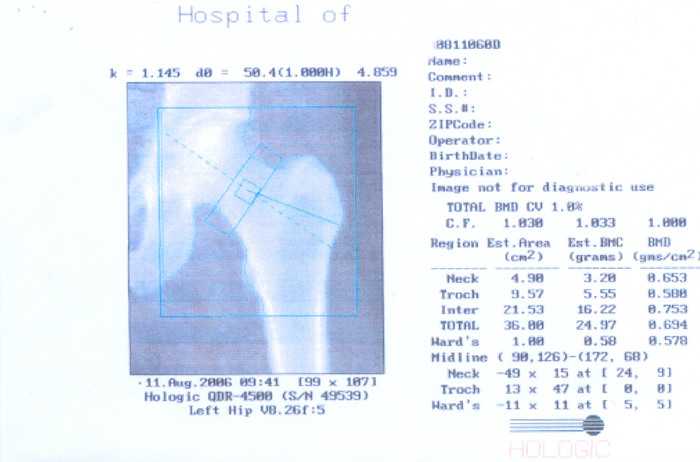 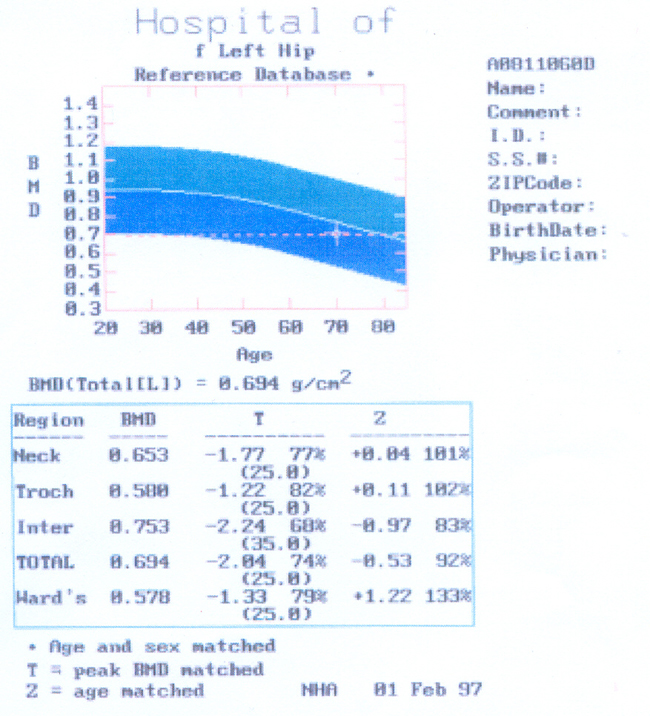
|
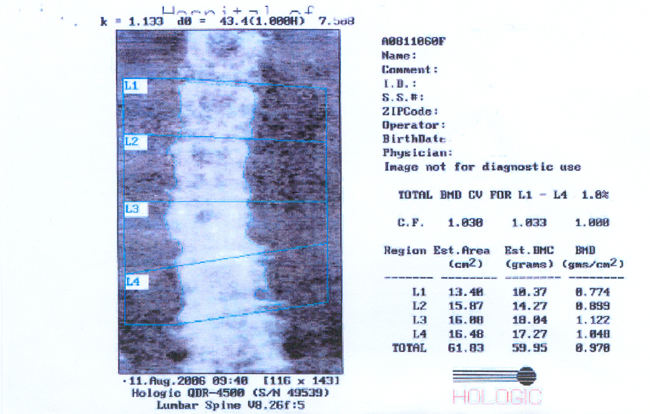 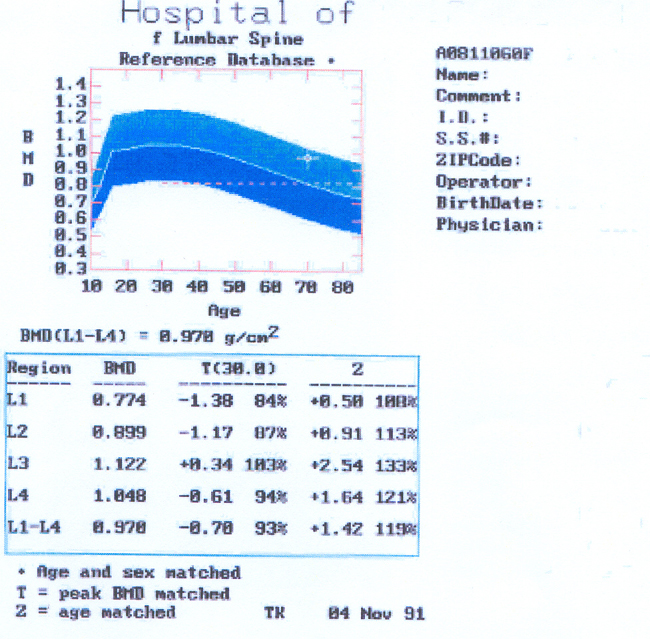
|
6.4 The women's interviews began with general lifestyle questions. It was not assumed that screening was important to the respondents, although they knew that the interview would focus on their experiences of health interventions for midlife women. They were asked how they had approached any decisions about the health interventions including the influence of their social situation and any feelings of vulnerability (Milburn 1996; Griffiths 1999), as well as any related health care encounters, since health professionals can have considerable influence on decisions about screening (Green and Wadsworth 1998; Griffiths 1999). In addition, their understanding of the health technologies at the focus of the project was explored. The health professionals were asked their views on health priorities for women at midlife in general, their own knowledge of the medical technologies and how they discussed them with women in the clinics. Interviews and clinical consultations were audio recorded, transcribed and coded in NVivo for ease of data retrieval. Analysis of the data was undertaken by the project team through a process of reading and re-reading the data, identifying key themes, relating the themes to social science and medical literature and then going back to the data. Although the selected data set is comparatively small, methodological strength is drawn from the combination of interviews and recorded consultations providing a triangulation of data which enabled the cross checking of accounts and afforded more understanding of the consultation process itself.
6.5 Interviews with the health professionals provided generalized accounts of their practice when working with bone densitometry, which we were able to consider alongside examples of what actually occurred. Similarly the women's interview data included their reflections upon the consultation, which provided both congruence and disjunction with the recorded event and enabled a fuller picture of the decision making process.
Perceptions of bone densitometry
7.1 Data from the subset of women's interviews and the broader sample of women's interviews, suggests that most women had internalised the imperative to keep well, which included taking full advantage of screening opportunities. Of those who had experienced it, the majority thought that bone densitometry could provide:- early diagnosis of osteoporosis
- a precise measurement of the risk of developing osteoporosis
- a key indicator of the potential need for intervention to prevent the development of osteoporosis, e.g. by taking HRT or bisphosphonates.
7.2 Consultation data from the subgroup confirm that clinicians were using bone densitometry screening in a process of risk assessment of the chances of developing osteoporosis based upon population probabilities, as part of preventative strategies. However, their women patients were waiting to be told whether they already had, or would develop osteoporosis, listening intently to what health professionals had to say about risk during the consultations. Data from their follow up interviews confirmed that clinicians' interpretation and discussion of the scan results was a major factor influencing women's decisions about treatment possibilities. Interviews with health professionals from across the study provided a different view, with many stating that a low bone density measurement was only one (albeit important) indicator of risk. However, the results of the bone scan provided in the form of a numerical measurement which was interpreted as above or below 'normal', loomed large in both the clinical consultations and women's accounts of their consultations narrated during separate interviews. Our analysis indicated that "where they are" on the graph becomes the focus of the consultation. On hearing the term risk factor, women seem to take it to mean that this particular health problem already has, or will affect them personally, rather than that it is a statistical probability. It appears that their belief that this type of screening technology can objectively measure risk by accurately predicting if and when they personally might develop 'thinning bones' is a key factor in women's decision making about treatment,. This includes taking HRT as an 'insurance policy', as the following extracts about bone densitometry screening indicate:
'For me it's been brilliant, err, it sort of stops something getting worse. I think it is a very effective service'.
Woman 62
I've always been quite aware of it since one of the nurses said I was a typical frame for osteoporosis and so I was pleased when she said I think I'll send you for a bone scan. I don't know whether I'll be pleased when I get the results back! But still, yeah, I'm quite conscious of osteoporosis and hopefully by taking the HRT it is one of the main reasons why I take HRT'.
Woman 48
7.3 Like the women in Howson's study of cervical screening (1998a, p204) they also perceived the screening itself as a form of insurance policy
'I go once a year .and I think you've got to have an awareness of this, I mean these things do happen, and a year is another year on, and I'm not sure quite what's happening inside my body, whether the things are. You see with bones you don't know whether they getting any weaker or not'.
'..(bone densitometry gives), peace of mind, the knowledge of what's happening, rather than the uncertainty of not knowing what's happening'.
Woman 64
'And then she [doctor] suggested I went and had the bone density checked, which I did, and it wasn't sort of very good at that point, it was just teetering, like teetering off the bottom end of normal and from that point of view I was aware that the HRT should help that, and prevent or reduce the risk of sort of osteoporosis. It was really only from that point of view that I decided to take it.'The last interview extract illustrates the woman's belief that being outside of, or on the lower end of the designated 'normal' zone indicated a risk level that she was uneasy about.
Woman 61
7.4Another woman who had been taking HRT for a number of years after advice that it would alleviate menopausal symptoms but who had now stopped taking it, sought regular access to the bone densitometry service for re-assurance that her bones were still within the 'normal' range.
'These examinations and scans and that it's marvelous because you know these parts of your body (laugh) are OK. You know, it gives you peace of mind'.Our data also suggests that after screening, some women who had 'healthy bones' became anxious enough to seek preventative treatment against osteoporosis:
Woman 53
'I went to have that (bone density scan) when I was just 51 and I was thinking, oh dear, ought I to go on HRT. I went and had it and they said the results were normal. When I probed they were actually very, they were actually lower than the average for the age range. The age range was actually 51 to 59. And I said, I don't call that average because I've got all that way to go up that age range, I'm not entirely happy with that although you say it's average. You know to my mind, to be below it, when you're at the young end of the age range, wasn't that good. So I spoke to the doctor and said, look maybe I should go on HRT '
Woman 04
7.5 What is striking about this extract is the image of a continuum from normal or average to at risk for her age range one that directly corresponds with the use of a population based statistical graph. This woman manages to insert herself into the relevant age group but appears to over interpret her individual risk, despite having been told by the health professionals that she is within the 'normal' range, she opts for intervention in the form of HRT 'just in case'. A similar strategy was also adopted by another woman after listening to a consultant's narrative about 'investing in your bones'. She described opting for HRT as a 'pension plan' to guard against the insecurity of the future when osteoporosis might become a health problem:
Patient: Yes, I know what you're saying.... It's long term
Dr: but it's an investment now err and as I say HRT....
P: It's like a pension plan (laughter)
D: It's investing for the future so, exactly
Consultation 01
'It can see into your bones'
8.1 Another important factor in persuading women that bone densitometry results were key to their decision making was their belief that the technology provided a clear image of thinning bones. The following extract is from a consultation between a radiographer and a woman attending for a bone scan.Radiographer: Yes (bone scanner) it's going all the way through and the picture I get on the screen here is, as each time it goes across your body it produces one line of the area that we're scanning.This extract provides a vivid example of bone scanning as a technology producing pictures of what Reventlow (2002) has referred to as the 'bone mass body,' drawing upon Scandinavian research on women's experiences of osteoporosis:
Patient: Oh right
R: And it's just a whole load of jigsaws that build up a picture. It shows me how much mineral is in your bones. I'm doing your hip, we know how much you should have for your age, sex, ethnic origin, what is normal for your age, so just compared with the normal data.
P: Oh right, so it's just the mineral content?
R: yes, measuring how much calcium (is) in your bones
P: Oh right
R: Now, this result will be with your GP in two weeks time.
Consultation 49
8.2It is not part of the radiographer's role to interpret the reading, such interpretation falls to a doctor, but the above extract illustrates the important impact that other professionals' informal comments on the scanning process might have, together with their perceptions of the key role played by the scan result. Communicating the result in 'pictures of your bones' appears to help women interpret its meaning but paradoxically, also contributes to them interpreting what are actually risk population probability calculations, as predictions of their own future risk, as the following extract shows:.
Dr: Now what the results have shown is this, is that the bone density, the thickness of the bones is a bit lower than average.
Patient: Right
D: And just to put it into pictorial context, here is the scan (and) here (on the graph) you can see the blue band is the normal range.
P: Yes
D: And this little box here represents the bone density measurements of three vertebrae, it's an average result, and as you can see it is a bit lower than average isn't it? So, your bones are a little bit thinner and therefore they are more likely to fracture for any given trauma or injury.
Consultation 61
8.3 What the doctor does not say, but the woman can probably see, is that a 'low average score' is nearer the risk range indicated outside of the blue band. Although the technology cannot speak for itself, this exchange provides an example of a situation when, as Brown and Webster (2004) argue, 'the body is made mobile, is broken up and becomes more, or less, a physical object' (p49), almost disconnected from the woman's experience of it. These women appear to understand the technology as providing a 'window' into their body, through which experts can assess the state of their bones. Scandinavian research on older women's experiences of osteoporosis ( Reventlow, Hvas et al. 2004 ) has suggested a similar idea where women come to understand themselves as bone mass bodies through the process of bone densitometry. Although Reventlow questions whether making previously hidden processes visible for the sake of prevention is empowering, since it appeared to leave many of the women in her study uncertain and afraid of this 'silent disease' which might strike them without warning.
8.4 A number of the women in our study shared this insecurity, although most were positive about the bone densitometry service. Few of the women included in our study had osteoporosis, with most considering intervention to prevent a future risk rather than building up currently brittle bones, but the line between future and current risk seems very blurred:
Interviewer: So, can you tell me what you know about screening through the bone densitometry service?
Patient: 'Naturally, it err, it tells you the bone density and err whether you've got osteoporosis or not, or what degree you're at, and it's very important and it is a very good screening process'.
Woman 60
Making Risk Visible: Interpreting the technological result through an expert
9.1 Interpreting risk and reducing uncertainty are part of clinicians' everyday practice which according to Ruston (2004) leads them to communicate certainty as calculable and bound up with control over knowledge. In the case of bone densitometry, the clearest information that they can offer is what Edwards and Elwyn (2001) have described as 'subjective probability'. This involves the health professional in digesting a variety of clinical information and other data drawn from many sources and applying it to his/her individual patient. The advice they give is rarely based upon a simple reading of the technological result. However, as Alaszewski et al. (2000) have noted, doctors given the same information often draw different conclusions and make different decisions. Also the interaction between the women and the practitioners in our consultations demonstrated the reaching of a compromise between different needs and priorities. Clinical protocols are not uniformly applied but instead are shaped by the relative importance of social, ethical and clinical factors.9.2 The following extract is from an interview with a woman who described actively seeking expert advice about treatment. It illustrates a number of the issues discussed so far in this paper, including women wanting to take advantage of all screening opportunities for preventing health problems and a belief in the technology as giving a result that can provide certainty about preventing osteoporosis:
Patient: I had been reading about it (osteoporosis) and thought; you know maybe you should have something done. I believe in having anything done that's available to make your life better and for the future, you know if there's anything gonna go wrong, try and stop it before it starts. So when I went into my GP, I just asked if I could have it, could I have a scan and she wrote off then and it started from there really.'Interviewer: So did they find that your bone density was low'?
P. 'It was borderline umm so which is why, and it got better being on the treatment (HRT) but then, as you get older, obviously it goes down anyway so, the last scan I had it was, still up slightly but it wasn't as good as it had been previously but that's because of the age thing I think. So I'm, quite happy on it, and I think I feel, psychologically you feel better if something is being done (laughter) you know, just to stop these things happening.'
Woman 67
9.3 When asked about her understanding of the reading, it is clear that she puts her trust in the professional to interpret it, translate it into user friendly language and advise her on treatment as the follow extract illustrates:
I. 'Ok. So, what is your understanding of the technological result'?P. 'I suppose I just understand, or, I just trust that what they are reading and what they're saying on the machine is right. I can just take note, I can just be advised by what the, whoever's reading them, what this tells me'.
Woman 67
9.4 This trust in health professionals to interpret the results of tests was found in the wider study also. Although the difficulty that health professionals have in interpreting statistical probability has been well described (Gigerenzer, 2002), our data illustrates the power of the 'expert' in a clinical setting. The following extract illustrates how the use of 'triangulation' enabled us to gain deeper insight into the decision making process. In the clinic, the following exchange occurred:
Patient: Do you think that I've got osteoporosis then now, is that what you're saying to me?In the follow-up interview with the woman, it appears that she had interpreted the 'falling' of the bone density as an indication that she currently had osteoporosis, despite the assurances from the consultant that at that time she was fit and well:
Dr You haven't at the moment, as measured.
P No, no
D But the results are dropping You're perfectly fit and well, in good general health. At the moment the results are normal, you have normal bone mineral density, but err after about 10 years it's going to drop into the below normal range, you can't be certain, but it's predictable.
Consultation 01
'I do feel that a lot more women should be able to have the bone screening. I do think that would be very important because of the risk of osteoporosis, because I'm probably very lucky that they've found mine.
Woman 60
The Clinical Encounter
10.1 The presence of the technology and what most women assumed to be precise 'objective' results seemed to heavily influence the dialogue in the clinical context. The fact that the key decision making takes place most often within a status ridden, clinical context, may make it difficult for women to resist the promise of technology (Brown, Rappert et al. 2000). The computer generated images of bones provided by the DEXA scan appear to illuminate the potential level of risk involved, rendering it visible enough to be shared with women in the process of interpretation by clinicians. This creates a new view of the body, one which is fragmented, an object of observation (Reventlow 2002; Brown and Webster, 2004), and a source of anxiety or danger for the women. In this context the bone scan appears to illuminate what has hitherto been an uncertain, invisible risk; embedded within the health professional's narrative about future health risk, it becomes one of what Haraway (1990) refers to as 'the crucial tools re-crafting our bodies'(p205). Applying this concept helps us to understand the suggestive power and importance of the DEXA scan result within the type of doctor-patient narrative typical of a consultation in a bone clinic. In the following extracts from two separate clinical consultations, a consultant is discussing potential changes in each woman's bone mineral density.Dr: And just to show you this, it's probably easier to sort of eyeball it than sort of discuss it, here's the measurement of the lumbar spine here shown on this graph and you can see your value is err this little box
Patient: Mmmh
D: The blue band is the average result for the population,
P: Right
D: Okay, so you can see there that your value actually is just bang on the average
P: Good
Consultation 58Dr: ..there has been a fall in the bone density measurements between '95 and '99 and the fall has occurred at both sites (of the body).
Patient: Yes
D: Now of course you would expect a reduction of bone density as we get older because that's the way we are.
P: Yes
D: Our density tends to drift down as one gets older but the values in relative terms are lower than um the average of a person of your age
Consultation 60
10.2 Three things are worth commenting upon here, firstly when the doctor refers to 'our density' and 'as we get older' he is referring to the 'normal population'. He invites the first patient to look at the graph which plots her individual measurement against the average for her age. Secondly, the graph is clearly represented as a technological artefact which 'speaks for itself', articulated within the language and meaning of the medical context, rather than the measurement being translated into everyday language that might be more readily understood. Finally, and more generally, our data from women having bone densitometry indicates that informing them that their bone mineral density readings were below 'normal', appeared to encourage them to take medication:
Dr: you know it (bone mineral density) shot up when you started the Kliofem, ...the HRT, and you've maintained that response, it's gone up even more, it's gone up another 4 or 5 per cent.
Patient: Excellent
D: which is ...., an excellent response to the HRT...and it's had the demonstrable effect on your bones,
P: Yes
D: your results are now in, are both in the normal range anyway.
P: Good
D: so, you have no increased risk of fracture,
P: Good
D: current medical advice is you can stay on (the HRT); ....the benefits of HRT are greater than the risks of up to, for up to ten years of treatment.
Consultation 64
10.3 Whilst it may be true that the woman's bones are within the range of 'normal', and that based on population evidence, staying on HRT was considered safe, this does not help the woman know if she will develop problems associated with taking the HRT. As we now know from research results published after the fieldwork was undertaken, the risks of taking HRT for 10 years or more are higher than previously supposed (Writing Group for the Women's Health Initiative Investigators, 2002; Million Women Study Collaborators, 2003). However, presenting the results in the apparently 'objective' language of graphs which can be emphasised as visual images, serves to elevate their status, and convinces the woman that continuing to take HRT is the appropriate course of action.
10.4 Although most health professionals in our study were aware of the limited usefulness of bone densitometry readings (Griffiths, Green and Bendelow, 2006), the readings nevertheless assumed an apparently objective, scientific measurement or 'result' within such clinical settings. Transforming the result to the level of the individual is not only difficult (Griffiths, Green and Tsouroufli, 2005) and without meaning, but could also be dangerous, for as Lauritzen and Sachs (2001) argue 'subtle boundaries between what is considered healthy and unhealthy or harmful and safe are negotiated and communicated together with the general norms that are valid for the population as a whole' (p514). As we have demonstrated earlier in the paper, some women whose bone mineral levels were recorded as well within the 'normal', opted to take medication 'just in case', and for 'peace of mind', seemingly related to the availability of the bone screening process and a common perception that it could detect early signs of disease.
10.5 The next extract from an interview with a consultant, also demonstrates the priority assumed by the scan result as a deciding factor in enforcing the (actually unclear) level of individual risk. In response to an interview question about whether he thought that bone densitometry was a good thing, one consultant said the following:
'Basically, yes. No test in medicine is perfect. What bone densitometry has been used as is a definition. Like most things in life, when you study it, it all disappears into the detail, but people want simple answers...we (medics) accept a bit more complexity in terms of management and treatment...'
Doctor 28
10.6 The statement seems to indicate that he is aware of the mismatch between the certainty which patients seek from such a measurement and the fact that it is only one of several risk indicators, and also that health professionals are accustomed to managing uncertainty. We don't know where his idea that 'people want simple answers' comes from; it may be based on long experience or prejudice. However, when he puts this idea into practice within the formality of a clinical setting, the 'simple answer' will impact heavily upon the decision making process. This, coupled with a 'scientific measurement format', elevates the authority of the DEXA scan reading and leads to what could be described as blurring the boundaries between socially constructed, context specific knowledge and 'objective' technology.
Communicating risk
11.1 Data from our study indicates that the ways in which uncertainty is managed by health professionals within the clinical context clearly has an impact upon what women 'hear' in consultations and their subsequent decisions. Our practitioners were under pressure to communicate risk of osteoporosis as part of an informed, coherent narrative which enabled the women to make choices about possible treatments such as HRT, as indicated in the following extract from an interview with a bone specialist:Interviewer: 'Can you tell me how you view these health technologies and what your knowledge and experiences are of them at a professional level'?Dr: 'I see them as useful aids to influence the discussion between a patient and doctor, which if you like take a little bit of the wondering out of it, in other words they give a value or some indication of risk which is a little bit more useful than just a clear diagnosis so we give a, if you like, a number to the degree of osteoporosis a person has. So it does enable people to see where they are in the spectrum of other patients' results and prioritise it and make decisions about what they want to do based on an objective measurement, so I think it's the objectivity combined with the fact that actually there's quite a good technique in terms of reproducibility. In other words you can get the same result repeatedly and you can use it as a tool to guide and influence people to appropriate management decisions about them, lifestyle or medication changes they're going to undertake'.
(Doctor 27)
11.2 As argued earlier, the health professionals were aware that the frequency of an event in a population can only be a guide for use by individuals weighing up their position, it cannot provide certainty. Despite this knowledge, they did attempt to communicate the level of risk involved to individual women. As Casper and Berg (1995: 399) argue, 'in their practice, physicians confronted with a patient's problem attempt to transform it so that it meshes with their work routine', part of which is dealing with patients' questions about levels of risk. However, when risk takes the form of an unknown, symptom less, invisible condition like osteoporosis, anxiety appears to encourage women to interpret that risk with greater certainty than the screening tests provide.
Discussion
12.1 The role of bone densitometry for screening for future osteoporosis remains controversial and the medical profession is now less clear about the best medical intervention for osteoporosis (Cranney 2003) given recent research findings about HRT. Despite this, medical consensus still favours the use of medication such as HRT for women whose health professionals consider them to be at high risk. And as data from the study reported here shows, some medics and women themselves view this as a form of 'insurance' against osteoporosis. The women in our study actively engaged with the medicalisation process (Griffiths, 1999; Williams and Calnan, 1996), trusted the results of the bone scanning and in common with those in Reventlow's et al's research (2005) appeared to believe that the images produced by the medical technology involved revealed some 'truth' about their bones.12.2 Assessment of bone density provides a precise measurement to which health professionals and women seem to be able to confidently refer in predicting future risk of osteoporosis. However, a number of key questions need to be asked, including whether this confidence is justified and does it apply to prevention of bone fractures, the major consequence of osteoporosis? In addition, we need to cast a spotlight on the practice of bone scanning for prevention and in particular, the process of deciding which factors influence a judgement of 'high risk' and the role that technology plays in such decision making. Subjective concepts of risk are significant here; our data demonstrates the difficulties which health professionals have in interpreting and communicating complex scan results in language which the lay person can understand. Use of the terms 'risk' and 'normal', 'average' or 'borderline normal' introduce uncertainty and ambiguity into consultation discussions and appear to have influenced a number of women to take medication to prevent a medical condition before it emerged. Health professionals' use of visual images embedded within the screening technology to articulate and clarify individual levels of risk of osteoporosis, produced ambiguous meaning on several occasions and left women with degrees of uncertainty about exactly what was being checked. This finding is congruent with research on cervical screening (Kavanagh and Broom, 1998, Howson, 2001). Although the women in our study expressed confidence in the bone densitometry service and actively participated in the screening process, their narratives revealed incomplete understanding of the results. Poor quality information delivered within the stock phrases embedded within clinical protocols may have made it difficult for women to absorb complex technical information.
12.3 Key health professionals in our sample adopted a relatively unproblematic use of population based evidence in the co-construction of narratives of individual risk with women patients. In addition, technology (or rather perceptions of technology) represented as a tool for 'seeing into bones' i.e. bone densitometry, takes centre-stage within such decision making processes. The fact that this is only one part of the clinical assessment may not be what the women want to hear (Parsons, Beale et al. 2000), or how they interpret the consultation. It seems to be precisely because bone densitometry is understood as providing facts about their bones, and acting as a window into the body, that the scan result becomes such a pivotal factor in women's decision-making about the need for intervention in preventing osteoporosis. This is an interpretation in which the health professionals concerned are at best complicit and at worst misleading; in their failure to inform women that contrary to expectation and patients' desire to reduce uncertainty, bone densitometry readings can only suggest probabilities. It appears that health professionals felt that they were expected to make interpretations that provided certainty. The pressure of such patient expectations influenced their attempts to communicate complex information in the most coherent manner possible (Griffiths, Green et al. 2005), leaving uncertainty out of the picture and may have unwittingly encouraged women to over-interpret the certainty of the results.
Conclusions
13.1 This paper has drawn upon data from a qualitative study of midlife women's health focusing upon their experience of health technologies designed for screening for osteoporosis. Findings from the study confirm that most of them are closely engaged in risk avoidance. What is also clear from the women's interview data, interview data from health practitioners and from recorded clinical consultations, is that a major dialogue between practitioners and women patients concerns the management or avoidance of health risks. We have argued that midlife women making decisions about the need for medical interventions to prevent or ameliorate age related health conditions such as osteoporosis are encouraged to view their bodies as ' declining bone mass constructions' that need to be monitored for objective indicators of risk. Bone densitometry screening as a case finding prevention strategy is a well established part of current health policies and practices but we need to be wary of the taken for grantedness of its 'success' on the part of health experts and lay people.13.2 We have drawn upon social science perspectives on risk, the medicalization and surveillance of women's bodies and associated research on health interventions such as screening (Howson, 1998a; 1998b; 2001), to explore the significance of bone densitometry technology in health decision making practices. The paper has developed a framework which attempts to link the articulation of screening experiences to the clinical practices within which they are embedded. Data from our study demonstrates that women are heavily reliant upon health professionals to both unambiguously interpret the information given by technological interventions such as bone densitometry and communicate the results in terms of individualised health risk. This is a specific example of a much broader debate which Webster (2002) refers to as 'medicine as information', arguing that medicine is being increasingly informaticized alongside mounting levels of uncertainty about risk diagnosis and clinical understanding. Although the health professionals involved in the screening process were aware of the uncertain nature of the risks being discussed during consultations, most failed to effectively communicate this to their patients, creating instead a myth of certainty about a condition that is inherently uncertain (Griffiths, Green and Bendelow, 2006). In many of the consultations and women's interview responses it appeared to be the 'normal bones' discourse within a biomedical model that dominated, a discourse that was overlaid by representations of bone densitometry as a precise technology that could provide clear images of problem bones.
13.3 The paper has explored the centrality of the bone densitometry reading or result, in midlife women and health practitioners' decision-making about the potential risk of osteoporosis and subsequent discussions about types of intervention and treatment. Although the results are open to flexible interpretation, they seem to confirm the 'at risk' status of many of the women in our study who had received a bone scan. Within the health risk narratives characteristic of our recorded consultation data, the numerically-based result appears to assume centre stage in the discussion, leading women to over-interpret its significance. It encouraged women to view their bodies as bone-mass skeletons, that become progressively unstable with age; leading some women to internalise messages about the need for intervention even when their bone density levels were pronounced to be within the normal range for their age. Furthermore, our data illustrates that key health practitioners in the study became complicit in such decisions, not least by virtue of their failure to challenge such partial understanding. Perceptions of the DEXA scan results as objective, technological readings which can reduce uncertainty obscure the ambiguities and clinical uncertainties embedded within them. More research that includes an exploration of such uncertainties may provide the key to understanding the social processes through which health risk consciousness is formed.
Notes
1Concerns about women who have taken HRT long term have surfaced in relation to results of recent US clinical trials that confirmed a higher incidence of breast cancer among such women (Writing Group for the Women's Health Initiative Investigators (2002)). "Risks and Benefits of Estrogen Plus Progestin in Healthy Postmenopausal Women." JAMA 288: 321-333. These results are supported by a UK epidemiological study, Million Women Study Collaborators (2003). "Breast Cancer and hormone-replacement therapy in the Million Women Study." Lancet 362: 419-427.Until the publication of the 2002 HRT research results, use of HRT by women in the UK was rising. HRT was recommended in medical literature for the relief of menopausal symptoms, the prevention of osteoporosis and as an intervention to be considered for the prevention of cardio-vascular disease such as heart attacks, Ballard, K. (2002). "Women's use of hormone replacement therapy for disease prevention; results of a community survey." British Journal of General Practice 52: 835-837.2The bone mass measurement recommended by the World Health Organisation in defining osteoporosis is 2.5 standard deviations or more below the mean bone density for premenopausal women Wilkin, T., D. Devendra, et al. (2001). "Education and Debate: Bone densitometry is not a good predictor of hip fracture." BMJ 323: 795-799.
3 It is important to note that the majority of our fieldwork was completed before the publication of the 2002 results on increased risks associated with HRT use.
4The final report for the project is available at YORK website address and all data from the study is available for bona fide use via the Economic and Social Data Service Qualida: http://www.esds.ac.uk/qualida/ (accessed 07.05.04).
5This qualitative study involved semi-structured interviews, recorded clinical consultations and focus group data. 109 NHS consultations were recorded between women aged 45-64 years and their healthcare professionals including doctors, nurses and radiographers, in 6 general practices and 3 specialist clinics. Individual interviews were conducted with 58 health professionals and 98 women; the latter recruited from healthcare sites or community locations.
References
ALASZEWSKI, A. H. et al. (2000). Managing Risk in Community Practice Nursing, Risk and Decision Making. London, Bailiere Tindall.ARMSTRONG, D. (1995). "The Rise of Surveillance Medicine." Sociology of Health and Illness 17: 393-404.
BALLARD, K. (2002). "Women's use of hormone replacement therapy for disease prevention; results of a community survey." British Journal of General Practice 52: 835-837.
BECK, U. (1992). Risk Society: towards a new modernity. London, Sage.
BROWN, N. and Webster, A. (2004) New Medical Technologies and Society, Cambridge, Polity Press.
BROWN, N., B. Rappert, et al., Eds. (2000). Contested Futures: a sociology of prospective techno-science.
Aldershot, Ashgate.
BURROWS, R.,S. Nettleton, and R. Bunton., (1995) Sociology and Health Promotion: Health, risk and consumption under late modernism. The Sociology of Health Promotion. R. Bunton, S. Nettleton and R. Burrows, Eds. London, Routledge.
BUSH, J. (2000) 'It's just part of being a woman: cervical screening, the body and femininity, Social Science and Medicine 50:429-444.
CASPER, M. J. and M. Berg (1995). "Constructivist perspectives on medical work: medical practices." Science, Technology & Human Values 20(4): 395-402.
CONEY, S. (1991) The Menopause Industry: A Guide to Medicine's Discovery of the Mid-life Woman Auckland, Penguin Books,.
CRANNEY, A. (2003). "Treatment of postmenopausal osteoporosis." BMJ 327: 355-356.
EDWARDS, A. and G. Elwyn (2001). "Communicating and understanding risk." Quality and Safety in Health Care 10(1): i9-i13.
FOUCAULT, M. (1973) The Birth of the Clinic, London, Tavistock
GANNON, L. (1999). Women and Aging: transcending myths. New York, Routledge.
GIDDENS, A. (1991). Modernity and Self-Identity: Self and Society in the Late Modern Age. Cambridge, Polity Press.
GIGERENZER, G. (2002) Reckoning with Risk, London, Penguin.
GRAHAM, H. (1979) ''Prevention and health: every mother's business'', in C. Harris (Ed) The Sociology of the Family: New Directions for Britain, Vol. 28: 160-185, Keele, University of Keele, Sociological Review Monograph.
GREEN, E, Thompson D and Griffiths, F. (2002). "Narratives of Risk: women at midlife, medical 'experts' and health technologies." Health Risk and Society 4: 243-86.
GREEN, E. and G. Wadsworth (1998). Disintegrating bodies: an analysis of women's experiences of the menopausal body. Making Sense of the Body: Theory Research and Practice, British Sociological Association.
GREER, G. (1991) The Change: Women, Ageing and the Menopause, London, Hamish Hamilton
GRIFFITHS, F. (1999). "Women's control and choice regarding HRT." Social Science & Medicine 42: 469-481.
GRIFFITHS, F. E., E. Green, and M. TSouroufli. (2005). "The nature of medical evidence and its inherent uncertainty for the clinical consultation: the example of midlife women." BMJ.2005; 330-511.
GRIFFITHS, F., E. Green, and G. Bendelow. (2006). "Health professionals, their medical interventions and uncertainty: a study focusing on women at midlife." Social Science & Medicine 62 (5): 1078-1090.
HARAWAY, D. (1990). A Manifesto for Cyborgs: Science, Technology and Socialist Feminism in the 1980's. Feminism and Postmodernism. L. Nicholson. London, Routledge.
HOWSON, A. (1998a) ''Surveillance, knowledge and risk: the embodied experience of cervical screening''. Health 2 (2): 195-215.
HOWSON, A. (1998b) ''Embodied obligation: the female body and health surveillance'' In S. Nettleton, & J. Watson (Eds.), The Body in Everyday Life. London: Routledge.
HOWSON, A. (1999) ''Cervical Screening, compliance and moral obligation'', Sociology of Health and Illness 21: 401-425
HOWSON, A. (2001) ''Locating uncertainties in cervical screening'', Health, Risk and Society 3 (2): 167-179.
KAVANAGH, A.M. and Broom, D.H. (1998) Embodied risk?: my body, my self, Social Science and Medicine 46: 437-444.
LAURITZEN, S. O. and L. Sachs (2001). "Normality, Risk and the Future: Implicit Communication of Threat in Health Surveillance." Sociology of Health and Illness 23(4): 497-516.
LOCK, M. (1998) Anomalous Ageing: managing the postmenopausal body, Body and Society 4 (1):35-61.
LUPTON, D. (1995) The Imperative of Health, London, Sage.
LUPTON, D. (1998). Going with the flow: some central discourses in conceptualising and articulating the embodiment of emotional states. In S. Nettleton, & J. Watson (Eds.), The Body in Everyday Life. London: Routledge.
LUPTON, D. (1999). Risk. London, Routledge.
MARTIN, E. (1987) The Woman in the Body, Milton Keynes, Open University Press.
MILBURN, K. (1996). "The importance of lay theorising for health research and practice." Health Promotion International 11: 41-46.
MILLION WOMEN STUDY COLLABORATORS (2003). "Breast Cancer and hormone-replacement therapy in the Million Women Study." Lancet 362: 419-427.
PARSONS, E. P., B. Beale, et al. (2000). "Re-assurance through surveillance in face of clinical uncertainty: the experience of women at risk of familial breast cancer." Health Expectations 3: 263-273.
POSNER, T. and Vessey, M. (1988) The Patient's View, London, The Kings Fund.
PRIOR, L., F. Wood, et al. (2002). "Making risk visible: the role of images in the assessment of (cancer) genetic risk." Health Risk and Society 4(3): 241-258.
REVENTLOW, S. (2002). "From accident to diagnosis, cultural reponses to the risk of osteoporosis." Revista della Societa Italiana di Antropologia Medica Italiana Oct: 87-99.
REVENTLOW S., Hvas, L. and Malterud, K. (2005) Making the body visible. bone scan, osteoporosis and women's bodily experiences, Social Science and Medicine 62 (2006) 2720-2731.
RICHARDSON, J. C, Hassell, A.B et al. (2002). "I'd rather go and know": women's understanding and experience of DEXA scanning for osteoporosis." Health Expectations 5: 114-126.
ROYAL COLLEGE OF PHYSICIANS AND BONE AND TEETH SOCIETY (2001) Osteoporosis: Clinical guidelines for prevention and treatment. London, Royal College of Physicians.
RUSTON, A. (2004). "Risk, anxiety and defensive action: general practitioner's referral decisions for women presenting with breast problems." Health Risk and Society 6(1): 25-38.
TANNENBAUM, C, B., Nasmith, L. and Mayo, N. (2003) Understanding older women's health care concerns: a qualitative study. Journal of Women and Aging.15/1
SINGLETON, V. (1995) ''Networking Constructions of Gender and Constructing Gender Networks: considering definitions of women in the British cervical screening programme, in K. Grint and R. Gill (Eds) The Gender-Technology Relation, London, Taylor and Francis.
WEBSTER, A. (2002). "Innovative Health Technologies and the Social: Redefining Health, Medicine and the Body." Current Sociology 50(3): 443-457.
WILKIN, T., D. Devendra, et al. (2001). "Education and Debate: Bone densitometry is not a good predictor of hip fracture." BMJ 323: 795-799.
WILLIAMS, S. J., L. Birke, et al. (2003). Debating Biology: Sociological reflections on health, medicine and society. London, Routledge.
WILLIAMS, S. J. and Calnan, M. (1996) The Limits of Medicalization? Modern medicine and the lay populace in 'late' modernity, Social Science and Medicine 42: 1609-1620.
WRITING GROUP FOR THE WOMEN'S HEALTH INITIATIVE INVESTIGATORS (2002). "Risks and Benefits of Estrogen Plus Progestin in Healthy Postmenopausal Women." JAMA 288: 321-333.

